Following recent reports of blood donation-related prosecutions in Russia, Singapore, and the United States, the HIV Justice Network undertook desk-based research, collating and categorising all known country and jurisdictional laws that specifically criminalise blood donations by people living with HIV, and known prosecutions under these laws. We analysed these laws and cases using a global policy guidance and human rights law framework, informed by international and state-level scientific data assessing risks of transmission via blood transfusion.
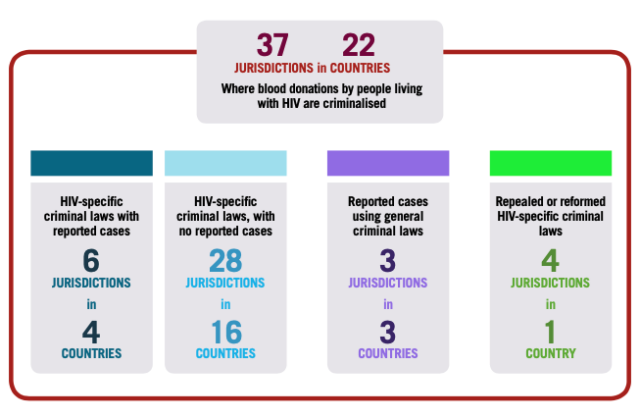
Bad Blood: Criminalisation of Blood Donations by People Living with HIV – written by Elliot Hatt and edited by Edwin J Bernard, based on research undertaken by Sylvie Beaumont, with additional input provided by Sarai Chisala-Tempelhoff and Paul Kidd (HIV Justice Network’s Supervisory Board); Sean Strub (Sero Project) and Robert James (University of Sussex – found that globally, 37 jurisdictions in 22 countries maintain laws which either explicitly criminalise successful or attempted blood donations by people living with HIV; or have related provisions which could be interpreted to criminalise this conduct; or have prosecuted people living with HIV who have donated blood under general communicable disease or other criminal laws. Notably, 15 jurisdictions in the United States (US) have laws which specifically criminalise blood donations by people living with HIV, while four US states – California, Illinois, Iowa, and Virginia – have repealed laws which previously criminalised this conduct.
Although prosecutions are relatively rare, we are aware of at least 20 cases relating to blood donation since 1987. Half of these cases have been reported in Singapore, including two as recently as 2021. The circumstances of these cases vary but most were of people who were unaware of their HIV status at the time of donation but withheld information relating to previous sexual encounters. Many only learned of their HIV-positive diagnosis when they were arrested. Reports of people who knowingly concealed their HIV-positive status when giving blood are rare, and from our analysis none involved donating blood with the specific intent to cause harm.
Preventing the transmission of blood-borne infection by imposing limitations on the donation of blood is an important and legitimate public health objective. Since the beginning of the HIV epidemic, certain groups – including, but not limited to, gay men and other men who have sex with men – have been subjected to restrictions on their ability to give blood. Sustained advocacy by gay rights organisations in many high-income countries has focused on the discriminatory nature of these so-called ‘gay blood bans’, highlighting significant advances in blood screening capabilities. This has led to a general softening of restrictions on blood donations for gay men in many of these countries – allowing donations with ‘deferral periods’, or allowing donations based on individual risk assessments.
However, this advocacy has generally not translated into the removal of HIV-specific criminal laws for donating blood, nor has there been a call for a moratorium on singling out people living with HIV for donating blood using non-HIV-specific general criminal laws – even though many of the same public health and human rights arguments apply to both the so-called ‘gay blood bans’ and to HIV criminalisation more generally.
The criminalisation of donors with HIV has primarily come about – and persists – due to both HIV-related stigma and homophobia and is not supported by science. The criminalisation of blood donations by people with HIV is a disproportionate measure – even if the aim of protecting public health through the prevention of transfusion-transmitted infection is legitimate.
There is no good reason for any country or jurisdiction to have HIV-specific criminal laws – whether they focus on blood donation or on sexual exposure or transmission. HIV-specific criminal laws are discriminatory and stigmatising, especially since people with other serious blood borne infections – including hepatitis B and C and syphilis – are not singled out with specific laws, nor for prosecution under general criminal laws.
Blood donation criminal laws focused on HIV should be repealed, prosecutions based on general laws should end, and instead science-informed measures – such as individual donor risk assessments and universal blood screening – should be relied on to protect the public against transfusion-transmitted infection.