A police officer in your article ( All in a night’s work, G2, 27 March) states getting HIV or hepatitis from uncapped needles as his biggest fear. Of all the risks police officers face, some highlighted elsewhere in the article, the risk of HIV infection is by far the lowest.
Germany: National AIDS Council releases powerful policy statement on HIV criminalisation
The German National AIDS Council – an independent advisory body of the Ministry of Health consisting of experts from the fields of research, medical care, public health services, ethics, law, social sciences, as well as people from the civil society – has produced a consensus statement on HIV criminalisation during consensual sex.
A press release issued yesterday by the Federal Ministry of Health states (unnofficial translation from German)
HIV infection has become a treatable chronic disease. In Germany, life expectancy with appropriate medical care is nearly normal. However, people with HIV still experience limitations, especially in everyday social life. They are often stigmatised and discriminated against in both the workplace and in the home environment. Criminal court judgments and their public perception play in a crucial role in this context.
- The National AIDS Council points out that the following medical factors should be assessed in criminal proceedings: HIV is difficult infection to transmit compared to other sexually transmitted diseases. The transmissibility of HIV is primarily related to viral load. In the first weeks after infection this is particularly high, and can amount to several million viral copies per milliliter of blood. After a few weeks or months, however, the immune system, usually controls the infection. Once viral load drops the body can keep viral load low for months or years before medication needs to be taken. During this time, the risk of infection is much lower than in the early phase of infection. Once the immune system weakens, generally antiretroviral therapy commences. With effective treatment, the viral load falls below the detection limit (viral load less than 50 viral copies / ml blood). If viral replication is permanently suppressed completely, according to current medical knowledge, HIV is not sexually transmitted. The risk reduction of successful antiretroviral therapy is at least comparable to the correct use of condoms. It is assumed that a large proportion of HIV transmission takes place during the early stages of HIV infection, i.e. at a time, when those who are infected are not aware of their infection, because an HIV antibody test can only show infection after a few weeks.
- Against this background, the National AIDS Council emphasises: A criminal examination of HIV exposure or transmission related to consensual sexual intercourse must be consistent with the medical facts. The decision whether or not the criminal liability of onward transmission can be assigned to the person with HIV cannot be made as a matter of routine. In fact, the determining factor are the circumstances of each individual case, especially the legitimate expectations of both sexual partners. In any case, in a short-term, consensual sexual encounter both partners are responsible for the application of protective measures, regardless of the knowledge or the acceptance of one’s own status and the status of the other person. Attributing either partner as perpetrator or victim is not appropriate.
Criminal proceedings regarding the transmission of HIV from consensual sexual intercourse do not contribute to HIV prevention. They can even be counterproductive in terms of the willingness of an individual to take an HIV test and in terms of open communication of sexual partners. In contrast, it is in the interest of the individual and society to increase willingness to take an HIV test.”
The full text of the statement (in German) can be found here.
US: New toolkit for lawyers defending HIV-related prosecutions now available
A new toolkit from the Center for HIV Law and Policy / Positive Justice Project, released earlier this month, provides a wealth of information for lawyers representing people living with HIV who are facing criminal prosecution based on HIV status.
The toolkit includes charts, articles, guidances, case law, legal analysis, scientific data and empirical citations, as well as quick-reference resources and links to longer reference materials.
The toolkit includes the following resources :
- HIV Criminalization Fact Sheet
- Guidance for a Legal Advocate Representing an HIV-Positive Client in a Criminal Exposure Case
- Guidance for People Living with HIV Who Are Threatened with, or Are Facing, Criminal Prosecution for HIV Nondisclosure or Exposure
- Case Law Index
- Legal Drafting Resources (featuring sample amicus briefs)
- Secondary Resources
- Sample Medical Expert Affidavit on HIV Transmission
- Chart: Comparative Sentencing on HIV Criminalization in the United States
- Chart: HIV, STIs and Relative Risks in the United States
- Chart: HIV and Chronic Disease in the United States
Although created primarily as a resource for lawyers, other advocates, as well as people living with HIV in the United States, are likely to find the toolkit useful.
Download ‘Ending and Defending Against HIV Criminalization: A Manual For Advocates Volume 2: A Legal Toolkit: Resources for Attorneys Handling HIV-Related Prosecutions’ from the Center for HIV Law and Policy here.
Consistent condom use in anal sex stops 70% of HIV infections, study finds, but intermittent use has no effect
An analysis by Dawn Smith of the US Centers for Disease Control (CDC) reported at the 20th Conference on Retroviruses and Opportunistic Infections (CROI 2013) on 4 March has provided the first estimate of the efficacy of condoms in preventing HIV transmission during anal sex since 1989.
UK: Updated guidance on HIV transmission, the law and the work of the clinical team now published
The British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASHH) have produced updated guidance on HIV Transmission, the Law and the Work of the Clinical Team.
This guidance is aimed at those working in the field of HIV medicine, especially clinicians, but will also be of use to general practitioners and people living with HIV who want to understand the legal and medical basis for some of their care decisions.
The guidance begins with a clear statement against HIV criminalisation:
BHIVA and BASHH believe that this use of the law is unhelpful and potentially harmful to public health and support UNAIDS recommendations to limit the use of criminal law and the Oslo declaration view that a “non-punitive, non-criminal HIV prevention approach” is preferable.
Covering the law in England & Wales as well as Scotland, the document aims to provide information and guidance on managing issues related to sexual transmission of HIV based on current scientific evidence. It applies generic ethical and professional principles but with a greater emphasis on providing a confidential environment in which extremely sensitive matters can be frankly and fully discussed. This enables appropriate care of people with HIV and benefits public health by encouraging individuals to access testing and treatment. Within this framework this document sets out the roles and responsibilities of health care professionals when caring for individuals living with HIV.
Consistent with the recent BHIVA and the Expert Advisory Group on AIDS (EAGA) position statement on the use of antiretroviral therapy to reduce HIV transmission, the guidance notes:
In most situations the appropriate use of antiretroviral treatment is at least as effective as condoms in preventing sexual transmission of HIV. This is accepted by the [Crown Prosecution Service of England and Wales] and [Scottish Crown Office and Procurator Fiscal Service] so it is likely that evidence showing that the defendant was taking effective antiretroviral treatment at the time of the alleged transmission may be used to demonstrate that they were not reckless.
The guidance also clearly states that healthcare professionals “must be mindful of their duty not to work beyond their expertise in legal matters. For people with HIV, advice must include the routes of HIV transmission and how to prevent transmission, with information about safer sexual practices, the use of condoms and suppression of viral load. Advice must be given in a non-judgmental way.”
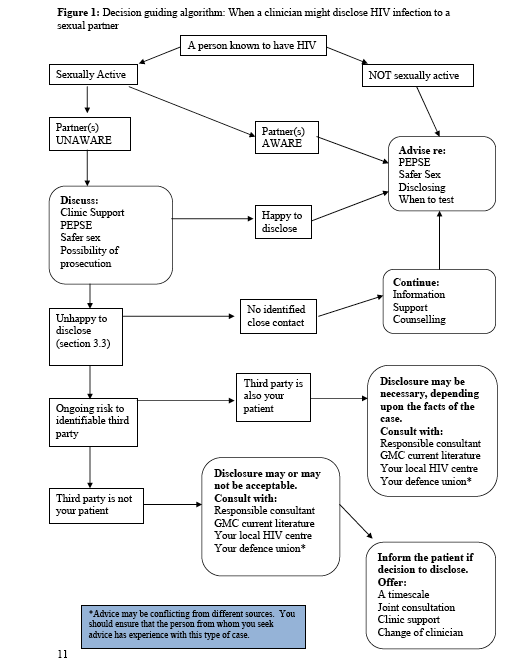
It also discusses issues of confidentiality, noting that “it is important when considering breaching confidentiality to weigh up all potential harms as there may be situations where disclosure of HIV status to protect a sexual partner results in considerable harm to an individual e.g. domestic violence. In situations where a health care professional believes that an HIV positive individual continues to put sexual contacts at risk their duties and subsequent action depend upon the type of contact.” See Figure 1 below.
The guidance also clearly states that “no information should be released to the police unless patient consent has been verified or there is a court order in place, except in very limited circumstances defined by the [General Medical Council].”
Importantly, it also notes that only individuals can make complainants to the police “and health care workers should remain impartial during discussions with patients.”
Finally, it provides clear advice to both help prevent transmission of HIV to sexual partners and to avoid prosecution for ‘reckless’ HIV transmission. Accordingly, people with HIV should do at least one of the following:
- Use a male or female condom fitted correctly along with water-based lubricant. Individuals doing this are unlikely to be seen as reckless for legal purposes. In the event of a condom split, it is advisable to disclose HIV status in order to support the partner’s decision whether or not to obtain post-exposure prophylaxis (PEPSE), which should be taken within 72 hours. The need for PEPSE will depend upon the type of sexual activity and the HIV viral load. An assessment of the risk should be undertaken by a clinician according to the BASHH PEPSE guidelines. Disclosure in these situations would suggest that the person with HIV was not reckless.
- Adhere to effective (suppressed viral load) antiretroviral medication. There is growing evidence of extremely low/minimal risk of transmission when plasma HIV is fully suppressed with the use of antiretroviral medication. In some situations an undetectable viral load can afford protection equivalent to or greater than that of condoms. A person with HIV is unlikely to be seen as reckless when relying on a suppressed viral load instead of condom use if they have been counselled accordingly by an HIV clinician or similar medical authority. It is recommended that this discussion is documented in the patient’s medical records.
In addition people with HIV should be advised that disclosure of HIV positive status to a partner before sex is important to support informed agreement around risk and safer sex behaviours. To avoid successful prosecution an individual who is not taking effective antiretroviral medication and does not use a condom must disclose their HIV status to sexual partners before sex takes place.
The entire guidance is reproduced below.
British public confused about how you get HIV
PUBLIC CONFUSED ABOUT HOW YOU GET HIV Nearly half (46%) of the general public wrongly think you can get HIV from being bitten, spat at or coming into contact with a discarded needle and underestimate the impact unsafe sex has on HIV transmission, a new survey[1] shows (14 Jan) .
Austria: HIV-positive man aquitted for ‘oral sex without ejaculation’ (Update)
Update: December 18th
A gay man on trial for allegedly exposing his ex-partner to HIV during ‘oral sex without ejaculation’ has been acquitted. The judge told the 37 year-old defendant that he had acted “entirely properly” according to Austria’s ‘safer sex’ guidance.
The case is covered in several Austrian newspapers, including Der Kurier and Der Standard, as well as the gay news portal, GGG.at.
It centred around a complaint following the end of a short-lived relationship between summer 2008 and spring 2009. The defendant was diagnosed HIV-positive during the relationship and waited several months to disclose this to the complainant. However, since he was counselled by his doctor that insertive oral sex without ejaculation would not expose his partner to HIV, and this was the only sexual risk at issue, his defence was that he had followed Austria’s ‘safer sex’ guidance.
Defence laywer, Helmut Graupner, told the court: “They are attempting to criminalise people who do exactly what the state wants them. This accusation is simply a scandal.”
(Under Articles 178 and 179 of Austria’s criminal code, disclosure is not a defence to potential HIV exposure, and so this case was not about non-disclosure, per se, but rather about whether the complainant was, in fact, exposed to HIV via oral sex without ejaculation.)
The complainant claimed on the witness stand that he had suffered mental anguish due to the fear of acquiring HIV, and he had brought the case partially because he wanted compensation for this.
However, Judge Eva Brandstetter agreed with the defence that ‘safer sex’ guidance was followed. It was “very clear that you behaved entire properly,” she told the defendant as she acquitted him.
The prosecution has until Friday to appeal the acquittal.
Original post: December 14th
Austria’s leading HIV and human rights lawyer has strongly criticised both Vienna’s prosecutorial authorities and the Austrian Ministry of Justice for allowing the forthcoming trial of an HIV-positive man for practising safer sex – namely, “oral sex without ejaculation”.
“The state must not criminalise HIV-positives for complying with the safer sex rules propagated by the same state“, says Dr. Helmut Graupner, president of Austria’s LGBT civil rights organisation Rechtskomitee LAMBDA (RKL) – who is also serving as counsel for the defendant – in a strongly-worded press release (see below). “This prosecution not only constitutes a serious human rights violation but also poses a considerable threat to public health.”
In addition Austrian MP Petra Bayr has tabled a parliamentary question to the Ministry of Justice concerning this ridiculous prosecution which asks:
- whether Parliament is aware of this prosecution;
- what it intends to do to ensure that prosecutors are aware of HIV tranmisssion risks and science;
- how it can justify HIV-related prosecutions under articles 178 and 179 of the criminal code when UNAIDS recommends against such prosecutions and asks whether Parliament will consider amending these articles to reflect up-to-date science; and
- what measures are being considered by the Justice Department to ensure consistent and science-based jurisprudence that promotes public health.
This is the second prosecution this year for perceived HIV exposure that, in fact, posed no risk whatsoever. In March 2012, a 17 year-old boy was convicted of HIV exposure after his 16 year-old girlfriend performed oral sex on him without him first disclosing that he was living with HIV. The judge said that even oral sex with condom would have been criminal as the use of condoms would not diminish the risk of infection.
The trial will take place this Monday, 17 December 2012, in room 307 at the Vienna Regional Criminal Court, Wickenburggasse 22, 1080 Vienna. Rechtskomitee LAMBDA’s press release notes that the trial is public which suggests that concerned HIV advocates could attend the trial to support the defendant (who cannot be named) and to show the prosecutor and judge that such prosecutions are out of step with science and do nothing for HIV justice.
The full Rechtskomitee LAMBDA’s press release can be downloaded here and is also reproduced below.
Austria: HIV-positive Man Prosecuted for Safer Sex
Trial next Monday in Vienna
An HIV-positive man stands criminal trial next week for practising safer sex propagated by the state and by the publicly funded aids service organisations. The prosecutor indicted him for “oral sex without ejaculation” (!), exactly what has been propagated as safer sex for decades.
The prosecution relies on Art. 178 of the Criminal Code (“wilful endangering of human beings by transmittable diseases”), an offence which for two decades had been used to convict persons (mostly women) even for sexual intercourse using a condom.
1997 the Supreme Court at last held that sexual intercourse with a condom is in accordance with the safer sex rules and no criminal offence (OGH 25.11.1997, 11 Os 171/97). And 2003 it was only after years of reopening-proceedings that the Graz Appeals Court to quash the conviction of an hiv-positive man for oral sex without ejaculation (Carinthian Oral Sex Case: http://www.RKLambda.at/news_safersex.htm). Already these days Austria´s then Minister for Health, Herbert Haupt, had stated, “that criminal persecution and conviction of hiv-positive persons for sexual contacts with hiv-negative persons in spite of them complying with the health authorities’ and aids-service-organisations´ safer sex rules run counter to effective hiv- and Aids-prevention (2313/AB XXI.GP, http://www.parlament.gv.at/PAKT/VHG/XXI/AB/AB_02313/).
Threat to effective HIV-prevention
Austria finds itself within the top ten worldwide regarding criminal conviction rates of hiv-positive persons (http://www.gnpplus.net/criminalisation/node/1262). Germany never had such a special offence and Switzerland recently restricted its law (which never had been as far-reaching as the Austrian one) to infection with malicious intent, thereby implementing a recommendation by the Swiss Commission on Aids (now: Swiss Commission on Sexual Health) (http://www.bag.admin.ch/hiv_aids/05464/12494/12821/, document for download on the right side). UNAIDS and the EU-Fundamental Rights Agency for years have been calling for a repeal of such criminalisation of HIV-positive persons and for restriction of criminal offences to intentional infection (http://www.unaids.org.fj/index.php?option=com_content&view=article&id=162:unaidsundp-policy-brief-criminalization-of-hiv-transmission-&catid=25:technical-documents&Itemid=74; http://fra.europa.eu/en/publication/2010/rights-based-approach-hiv-european-union, http://www.hivjustice.net/oslo/oslo-declaration/).
Accordingly the Austrian Minister of Justice in 2010 on the occasion of the Vienna World Aids-Conference had assured that Austrian criminal law would not criminalize sexual acts in accordance with the safer sex rules and declared that the prosecutors would be informed to this effect (4941/AB, 2 June 2010, http://www.parlament.gv.at/PAKT/VHG/XXIV/AB/AB_04941/).
Double game played by the (Minister of) Justice?
Nevertheless last spring a 17 year old juvenile has been convicted for oral sex (without the allegation of ejaculation) with the judge even claiming that the use of a condom would not have made a difference (http://vorarlberg.orf.at/news/stories/2523707/). And now in Vienna the prosecutor is indicting a man explicitly even for oral sex without (!) ejaculation, behaviour explicitly propagated by the health authorities´ and the aids-service-associations´ (http://www.aids.at/alles-uber-hivaids/wie-kann-ich-mich-schutzen/; http://www.aidshilfen.at/sie-haben-fragen-wir-haben-antworten; https://www.gesundheit.gv.at/Portal.Node/ghp/public/content/Safer_Sex.html).
The trial takes place next Monday, 17 December 2012 in room 307 at the Vienna Regional Criminal Court, Wickenburggasse 22, 1080 Vienna. The trial is public. Revealing the defendant´s identity in the media is strictly prohibited (§§ 7 & 7a Media Act).
Members of federal parliament have tabled a parliamentary question to the Ministry of Justice concerning this incredible prosecution (13275/J, 6 December 2012, http://www.parlament.gv.at/PAKT/VHG/XXIV/J/J_13275/).
“The state must not criminalise HIV-positives for complying with the safer sex rules propagated by the same state“, says Dr. Helmut Graupner, president of Austria’s LGBT civil rights organisation Rechtskomitee LAMBDA (RKL) and counsel for the defendant, “This prosecution not only constitutes a serious human rights violation but also poses a considerable threat to public health.”
Clear, concise interview on risk, legal literacy following Canadian Supreme Court decision
In a wide–ranging interview that poses difficult questions, Bob Leahy asks Toronto-based clinician/scientist Dr. Rupert Kaul about how can we interpret risk of HIV transmission in the age of undetectable viral load.
More criminalization, further marginalization: Supreme Court's HIV non-disclosure decisions create viral underclass |
This is the second in a series of blog posts about the recent Supreme Court of Canada decisions about the criminalization of HIV non-disclosure. See the first post here, in which we wrote about the perverse, negative impacts of the decision for women living with HIV.
US: Scott A. Schoettes of Lambda Legal outlines the battle being waged in U.S. courts over HIV criminalisation in POZ Magazine
Scott A. Schoettes is the HIV project director for Lambda Legal, a longtime legal champion of HIV-positive people and LGBT civil rights. He filed a brief in The People of the State of New York v. David Plunkett, an HIV criminalization case heard by the New York Court of Appeals, the highest court in the state.