Yesterday saw the release of an important new UK study, Keeping Confidence: HIV and the criminal law from service provider perspectives, which explores how HIV criminalisation impacts those who deliver health and social care services for people with HIV.
The report’s lead author, Dr Catherine Dodds, from Sigma Research at the London School of Hygiene & Tropical Medicine, said: “Although HIV health and social care professionals expressed diverse views about their potential role in such cases, they gave a clear sense that criminal prosecutions for the transmission of HIV would not improve public health. Instead, it was most common to hear descriptions of such cases leading to increased stigma, reduced trust between service users and providers, and traumatic consequences for those involved in such cases.”
Study co-investigator, Matthew Weait, Professor of Law and Policy at Birkbeck, Univerisity of London, said: “This important and innovative research demonstrates both the problems that HIV criminalisation creates for clinical and social care providers and the need for solutions at both national and regional level. Care providers working in HIV and sexual health are concerned primarily with the health and wellbeing of their service users – which is of course as it should be; but there is also evidence that criminalisation is compromising their work. Increased awareness and understanding of, and inter-organisational communication about, legal issues is critical, and Keeping Confidence makes practical recommendations as to how that work might be taken forward for the benefit of prevention and support.”
Roger Pebody from aidsmap.com does an excellent job of summarising the study and its findings in this news report:
The study explored how criminal prosecutions for HIV transmission in England and Wales are handled by those who deliver clinical, psychosocial and community support for people with HIV. The report paints a picture of professionals grappling with the difficulties of communicating complex legal information in an appropriate way for each individual. They must weigh up competing concerns and responsibilities, including their own patient’s health and wellbeing, the health of unidentified sexual partners and the legal liability of their own organisation.
Read more at aidsmap.com
The report was launched in central London yesterday at a one-day meeting attended by around 70 HIV service providers, representatives of most of the UK’s community-based HIV organisations, and people living with HIV.
Following presentations of the report’s main findings, a panel consisting of a health adviser, and representatives of community-based organisaton and a people living with HIV discussed the implications for them.
Ceri Evans, Senior Health Adviser at the West London Centre for Sexual Health, Chelsea and Westminster Hospital, highlighted that there may not be a ‘best time’ to inform a newly diagnosed individual of their new legal obligations. Athough she agreed that the post-testing counselling session may not be ideal, she noted that since the criminal law potentially covers all sexually transmissable infections, including genital herpes, and there is usually only a single oppportunity to provide counselling following a new herpes diagnosis, that information about the law might need to be provided to some patients sooner rather than later.
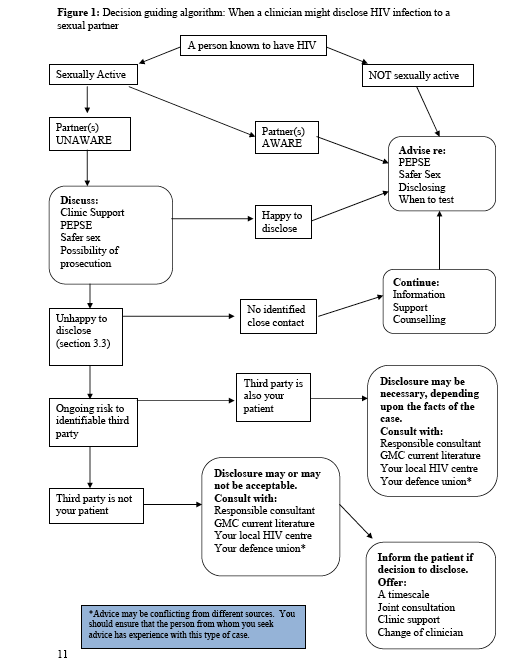
Of note, the report’s fieldwork, involving 75 providers of HIV health and social care services in England and Wales, was undertaken in the latter half of 2012. Since then, the British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASHH) have released an updated position statement on HIV Transmission, the Law and the Work of the Clinical Team which provides clinicians with information and guidance on managing many of the issues highglighted as problematic in the research. Lead author, Dr Mary Poulton, Consultant and Clinical Lad, Sexual Health and HIV, Kings College Hospital, London, outlined the main recommendations and provided case studies that illustrated how the decision-guiding algorithm regarding third-party disclosure might be particularly useful.
The rest of the meeting focused around discussing the report’s recommendations, which were as follows.
National recommendations
1. HIV service professionals will benefit from a single website or webpage that collates practical and accessible information about criminal prosecutions for the sexual transmission of HIV. It will need to be updated as new resources become available, and older ones are revised. New resources should be published as required in order to keep pace with clinical and scientific developments in the treatment of HIV that may impact on legal decision-making. The online resource can also identify the best sources of expert criminal legal advice where those are available.
2. A nation-wide programme of continuous professional development in the criminal law should be available to those who provide clinical and non-clinical HIV services. Topics covered should include: straightforward legal definitions and defence arguments, how and when to raise discussions about legal responsibilities, professional liability, communication skills development through the use of scenarios, and existing policy and practice models.
3. Key contacts with an interest in criminal prosecutions should be identified in each clinical and non-clinical HIV service organisation.This process should feed into the development of an updated list for the explicit use of disseminating information about information and training discussed in recommendations 1 and 2 above.The key contacts will also be utilised as the main organisational contact for the development and dissemination of resources to inform people with HIV about the law in this area.
Local recommendations
4. Existing professional guidance and associated documents should be discussed and adapted for local use. This will translate differently in specific settings, and it may lead to the development of local criminalisation policies or protocols, or values statements in some workplaces. At a minimum, such activities should strive for internal consistency on advice, facilitation and support.
5. Opportunities should be created for clinics and community-based organisations to exchange best practice as it relates to criminal prosecution for HIV transmission and to discuss where they agree and disagree on a conceptual level about the ethics of responsibility and public health in HIV prevention.
6. Alongside the development of local criminalisation protocols, all organisations will need to review their confidentiality policies, ensuring that they are accessible to service users, and compatible with internal agreements about criminalisation.
Whilst there was broad consenus regarding many of the recommendations, implementation will depend on various stakeholders collaborating, as well as sufficient funding.
Of note, currently only Australia has a website on HIV and the law aimed specifically at HIV healthcare professionals. The Australian Association of HIV Medicine (ASHM) online Guide to Australian HIV Laws and Policies for Healthcare Professionals covers civil, criminal and public health law, and also includes reference to national guidance on the Management of People with HIV who Place Others at Risk.
The entire day was filmed by the HIV Justice Network and video of the main presentations and final disussion outcomes will be available soon.